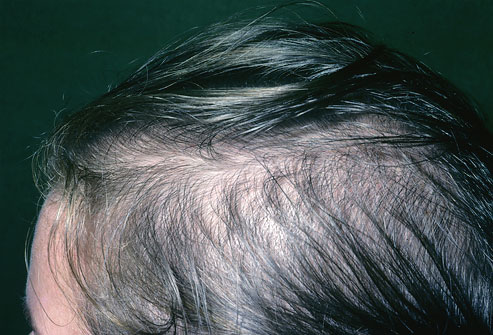
Female hair loss – why does hair loss happen to women?
Updated 2/7/21:
Although we mostly associate hair loss with men, women’s hair loss problems are also quite common. Many people believe hair loss only affects males. It is estimated, however, that more than 50% of females would experience noticeable hair loss. Female-pattern hair loss (FPHL) is the most prevalent cause of hair loss in women, affecting about 30 million women in the United States.
Female hair loss is even tougher to fight against than male hair loss since this topic has a lot less coverage in both print and online media. This is due to the unfortunate stigma involved with female hair loss. Women face a whole other set of circumstances that cause hair loss to be more traumatic because of societal pressures facing women and the pressure to appear beautiful. Hair loss in women is a condition that has to be treated with maximum seriousness and the first step is for the woman to acknowledge the problem and take steps to solve it. A proactive female hair loss treatment is one of your best bets since many doctors seem to ignore treatments for hair loss in women.
Hair loss in women is harder to treat than male baldness
Doesn’t sound good, but the brighter news is that the reversibility of female hair loss is a lot higher than with male patients. Finding the right female hair loss treatment should begin with eliminating all the potential underlying causes until the actual trigger is found. A woman’s hair loss is usually related to hormonal imbalances.
For example, an unbalanced response from your thyroid might cause different physical responses from your body. Hypothyroidism and hyperthyroidism, which are extreme and prolonged, can cause hair loss. Instead of different regions, the loss is diffuse and affects the entire scalp. The hair appears sparse uniformly. With effective thyroid disorder treatment, regrowth is normal, but it may take several months and may be incomplete. It is rare to cause hair loss due to moderate (e.g. subclinical) hypothyroidism or hyperthyroidism, or short-lived thyroid issues. Some cases of hypothyroidism and hyperthyroidism arise unexpectedly and are diagnosed early, whereas others may have been present before diagnosis for months or years. Some months after the onset of thyroid disease, hair loss due to thyroid disease becomes apparent. The long hair cycle is responsible for this. In such cases, paradoxically, thyroid treatment may be accompanied by hair loss, and thyroid medicine may be falsely blamed, leading to the cessation of therapy, which in turn may make hair loss worse.

Some pregnant women also experience some forms of hair loss. Several hormonal disorders, such as hyperandrogenism, thyroid gland diseases, and hyperprolactinemia, may affect reproductive periods in women. These endocrine disorders, as well as hypercortisolism and excessive secretion of growth hormone, both of which occur much less frequently, may lead to hair growth disorders, such as hirsutism, hair loss in female patterns, and other types of alopecia. Hirsutism is a common endocrine disorder that occurs in 5-10% of reproductive-age women and is characterized in females as excessive terminal hair in a male pattern that appears on women.
On the other hand, female hair loss is also likely to be triggered by menopause. Like hot flashes, a common symptom that occurs during menopause is hair loss. Most women who notice hair loss from menopause do not medically have anything wrong with them. Some women may experience more severe hair loss, known as female hair loss pattern (FPHL), where on the top and crown of the head there is thinning. Hair loss during menopause is most often due to hormone changes. When levels of estrogen and progesterone (female hormones) fall during menopause, this form of hair loss occurs. Such hormones enable hair to develop and remain strong. The effects of androgens (male hormones) increase as levels of estrogen and progesterone decrease during menopause. As a consequence, hair develops at a much slower rate and hair follicles shorten, resulting in thinner hair and eventually causing hair loss. A hereditary predisposition, elevated levels of stress, dietary deficiencies, and certain drugs are other factors that may lead to hair loss during menopause.
Dietary deficiencies
Dietary deficiencies are also possible culprits when it comes to female hair loss. People with hair loss also question if nutritional supplements will help restore hair growth or avoid further loss of hair. In reality, in the expectation that the supplements will benefit, many will begin dietary supplements without consultation. The unregulated supplement industry often capitalizes on the weakness of this population. While hair follicles are among the most metabolically active in the body, and calorie and protein malnutrition, as well as micronutrient deficiency, can affect hair growth, the ties are complex. Here are some supplements that can cause hair loss if they are deficient:
Iron
Iron deficiency (ID) is a well-known cause of hair loss and is the most common nutritional deficiency in the world. What remains unknown is what degree of ID will lead to the loss of hair. There are no definitive answers at this moment in regards to ID and hair loss. On a case-by-case basis, patients have to be analyzed to see what the optimum level should be.
Zinc
Zinc is an important mineral needed by hundreds of enzymes and multiple gene expression-regulating transcription factors. Although the exact mechanism of action is uncertain, the function of zinc as an integral component of multiple metalloenzymes critical for protein synthesis and cell division is one possibility. The role of zinc in the Hedgehog signaling pathway, a crucial element in the pathways regulating hair follicle morphology, is another possibility. However, minimal evidence is currently available on the effects of zinc supplementation on hair growth in those without a confirmed deficiency. A single patient with alopecia, without a specific deficiency, who experienced improvement following oral zinc therapy was identified in one study.
When considering supplementation in the absence of a known deficiency, a major point is that with excess supplementation, zinc toxicity can occur. Pressure, vomiting, and diarrhea are acute side effects, while chronic effects include iron interaction and decreased immune function.
Niacin
Pellagra (a disease caused by a lack of the vitamin niacin (vitamin B3)) contributes to the well-known triad of photosensitive dermatitis, diarrhea, and dementia due to a deficiency of niacin. Another frequent clinical finding is alopecia. Pellagra became scarce in many developing nations until the introduction of food fortification with niacin. In developing countries, alcoholism is now considered the most common cause of pellagra. Other causes include conditions of malabsorption or drug-induced cases, such as isoniazid. No studies on niacin levels in patients with hair loss alone were found in a study of the literature.
Fatty Acids
Deficiency of linoleic acid (omega-6 fatty acid) and alpha-linolenic acid (omega-3 fatty acid) in polyunsaturated essential fatty acids can result from inadequate parenteral nutrition and malabsorption disorders such as cystic fibrosis. Hair modifications include the loss of hair on the scalp and eyebrows, as well as hair lightening. Limited information concerning supplementation is, however, available. The topical application of safflower oil, high in linoleic acid, resulted in hair growth in one patient with essential fatty acid deficiency. Although findings were reported from a study using a supplement, limited conclusions could be drawn, as multiple fatty acids and antioxidants were mixed in this supplement.
Selenium
Research on selenium deficiency and alopecia in humans is minimal. In a boy, one case report identified sparse hair, which improved following dietary supplementation. Given the small number of human studies, it is shocking that some supplements for hair loss are advertised as selenium-containing. As selenium toxicity from dietary supplementation is well known, this is worrying. As well as blistering skin lesions, gastrointestinal symptoms, and memory difficulties, toxicity can result in generalized hair loss.
Vitamin D
Inadequate sun exposure, dark skin, obesity, gastric bypass, and fat malabsorption are risk factors for vitamin D deficiency. One analysis of eight women with telogen effluvium or FPHL found that serum levels of vitamin D2 were significantly lower than control levels. In addition, with increased disease incidence, vitamin D2 levels decreased. However, there is a lack of evidence concerning the impact of vitamin D supplementation on hair loss.
Vitamin A
Vitamin A is a group of compounds comprising carotenoids from retinol, retinal, retinoic acid, and provitamin A. Dietary vitamin A has been shown to stimulate hair follicle stem cells in murine studies, although its role is recognized as complex and precise levels of retinoic acid are needed for optimal hair follicle function. While deficiency has not been associated with hair loss, elevated levels may be a concern, on the other hand. In fact, one study showed that the reduction of vitamin A in the diet in a mouse actually delayed the onset of hair loss.
Vitamin E

Tocotrienols and tocopherols belong to the family of vitamin E and are important antioxidants. Deficiency results in hemolytic anemia, dryness of the skin, and neurological findings. Deficiency in vitamin E is rare but can occur with disorders of fat malabsorption. There is little information in the literature on the effects of supplementation with vitamin E for hair loss. One analysis of 21 volunteers receiving tocotrienol supplementation (100 mg daily of mixed tocotrienol) reported a substantial improvement in hair count relative to the placebo community.
Folic Acid
In leafy greens, folic acid is present and many foods are fortified with folic acid, rendering deficiency uncommon. Deficiency results predominantly in megaloblastic anemia, without the appearance of hair loss. Compared to controls, no substantial difference in serum folate levels was seen in 91 patients with diffuse hair loss. In fact, further analysis of 200 women with chronic TE found that 28.5% had elevated serum folic acid, although the study methodology was not used and minimal conclusions could therefore be drawn.
Biotin
Biotin, or vitamin H, a deficiency is rare, as usually, intestinal bacteria are capable of producing sufficient biotin levels. Deficiency is seen in cases of antibiotic use, where there is a reduction of gastrointestinal flora needed for the production of Biotin. In the absence of a deficiency, no clinical trials have demonstrated effectiveness in treating hair loss with biotin supplementation. In spite of this, biotin is present in numerous hair loss supplements sold to customers. Since biotin has shown beneficial effects in the treatment of brittle fingernails, this marketing strategy may have been selected.
Amino Acids and Proteins
A lack of the proper level of proteins can lead to hair changes that involve hair thinning and loss of hair. The role of L-lysine, an important amino acid that may play a role in iron and zinc uptake, was examined in one study. In some women with chronic telogen effluvium who did not respond to iron supplementation alone, the addition of L-lysine to iron supplementation resulted in a substantial increase in the mean serum ferritin concentration. Although interesting, the data available is small, and the function of L-lysine should be further investigated. No strong conclusions on the role of supplementation in hair loss can be drawn in terms of other amino acids and proteins. While amino acid and protein supplement studies have been released, a variety of nutrients are formulated and it is therefore uncertain what role, if any, amino acid and protein supplementation can play in the absence of a known deficiency.
Antioxidants
Compounds that can neutralize reactive oxygen species (ROS) and avoid oxidative harm are called antioxidants. Many substances, including zinc, selenium, and vitamins A and E, as mentioned earlier in this article, as well as vitamin C and polyphenols, can be classified as antioxidants. Hair loss has been associated with oxidative stress. High doses of antioxidants have been shown to protect against reactive oxygen species (ROS). Although dietary antioxidants play a key role in strengthening our endogenous antioxidant system, the balance between oxidation and antioxidation can actually be interrupted by high doses of antioxidant supplements. In contrast to large doses found in supplements, compounds in plant foods, such as fruits, vegetables, and grains, may be safer and healthier.
(Always consult with a Doctor before taking new supplements)
In conclusion
As you can see there are many potential triggers for hair loss in women. Consult with your doctor and find a good female hair loss treatment. An educated female hair loss specialist will have a much better understanding of your problems. Try to present your doctor with a complete list of potential hair loss triggers, this will save both of you some time and will increase the chances that you get the best hair loss treatment.
Some physicians, however, do not have a very good understanding of female hair loss, even though they are experts in male baldness. It is your duty to ensure that they follow the right recommendations for hair loss in women with the proper medication and healing methodology. Good luck in your journey to find an effective treatment.
Sources:
https://my.clevelandclinic.org/health/diseases/16921-hair-loss-in-women
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7432488/
https://www.btf-thyroid.org/hair-loss-and-thyroid-disorders
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5315033/
https://nwhn.org/menopause-hair-loss/
=======================================
© 2012-2021 by BaldTalk.com. All rights reserved. No part of this document may be reproduced or transmitted in any form or by any means, electronic, mechanical, photocopying, recording, or otherwise, without prior written permission of BaldTalk.com.